


A Comprehensive Approach
The need for a unified approach to diagnosing and treating addictive illness is underscored, as one considers the enormous expenditure of government funds, in research, prevention, education, treatment, interdiction, and incarceration, related to substance abuse and other addictive illness in the United States. “Drug abuse and addiction are a major burden to society; economic costs alone are estimated to exceed half a trillion dollars annually in the United States, including health, crime-related costs, and losses in productivity,” Nora Volkow, MD.
The “Syndrome Model” of addiction has emerged in recent decades, as a significant advancement from the monoculture of the “disease concept”, and other traditional responses to addiction (i.e. the moral deficiency of a person, or the inherent property of a substance or activity). Howard Shaffer, PhD, CAS, et al, makes a strong case for a new understanding of addictive illness, as a syndrome, “A cluster of symptoms and signs related to an abnormal underlying condition.” The Syndrome Model captures the complexity of addiction, suggesting that some shared symptoms are present in every expression of the syndrome (tolerance and withdrawal), while other manifestations of addiction have unique symptoms (cirrhosis with alcohol dependence, STDs with sexual addiction).
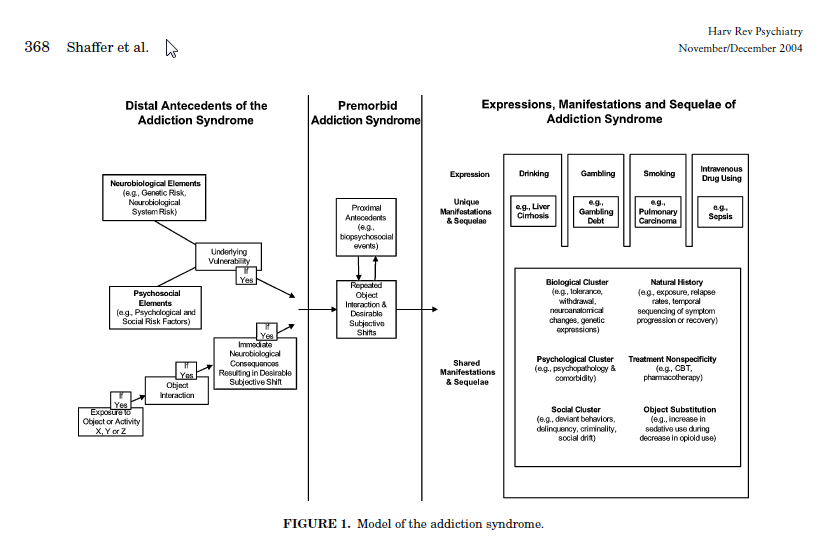
Shaffer conceptualizes addiction's origins in “distal antecedents”, both neurobiological and psychosocial, generating a “premorbid addiction syndrome.” Biopsychosocial events, or “proximal antecedents” advance the addiction syndrome from the premorbid phase, through “repeated object interactions” with “desirable subjective shifts” that constitute euphoric experience. Shaffer describes the observable symptoms of addiction in overlapping sets of “shared” and “unique” “manifestations and sequelae” that confirm the presence of substance and behavioral addictions. This convergence of multiple precursors produces the “perfect storm” of addiction… a syndrome with common features observed across all cases, and individual differences that emerge from this maelstrom of complexity.
Among the significant implications of the Syndrome Model of addiction, Shaffer suggests that the study of addictive illness will yield “objective diagnostic criteria”, in contrast to the “consensus-based” structure of the DSM, with its inherent lack of validity. Shaffer decries the current prevalence of “object-specific” treatment approaches, noting that “80 to 90% of individuals entering recovery from addiction will relapse within the first year of treatment.” Guiding the addictions field towards more comprehensive interventions, Shaffer observes that “the most effective addiction treatments are multimodal ‘cocktail’ approaches that include both object-specific and addiction-general treatments.” Shaffer concludes that, “Finally, with its emphasis on etiology, an addiction syndrome model encourages the use of diagnostic “gates.”
The GATE Model supports a dynamic understanding of the etiology and treatment of addiction, advancing the dialogue from the static representations of traditional 12-step approaches and the “disease concept” to a user-friendly, interactive, graphic representation of complex dynamics described in the Syndrome Model of addiction.
